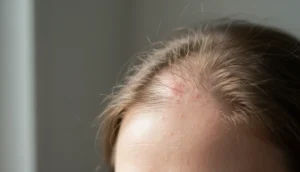
Experiencing hair loss after operation can be unsettling, especially when you’re focused on healing from a major procedure. This article explores the physiological reasons behind post‑surgical shedding, the influence of anesthesia and rapid weight changes, and practical steps you can take to support healthy regrowth. According to dermatological studies, up to 30 % of patients notice noticeable thinning within the first three months following surgery, making it a common yet often misunderstood concern.
We’ll break down the science of telogen effluvium, examine how weight loss and nutritional deficits amplify shedding, and identify warning signs that suggest a deeper issue. Whether you’ve undergone a cosmetic operation, bariatric surgery, or a routine medical procedure, understanding the mechanisms at play will empower you to take proactive measures.
By the end of this guide, you’ll know when the hair loss is temporary, when it may require medical attention, and how a specialized hair restoration clinic like Gold City Hair can help you restore confidence through advanced techniques such as FUE and DHI.
Understanding Post‑Surgical Hair Shedding
The most common form of hair loss after operation is telogen effluvium, a temporary shift that pushes hair follicles into the resting phase. This reaction is typically triggered by physical stress, hormonal fluctuations, and the body’s response to anesthesia.
Telogen Effluvium Explained
During a normal hair growth cycle, about 85 % of follicles are in the anagen (growth) phase, while the remaining 15 % are in telogen (resting). A major stressor—such as surgery—can cause up to 30 % of hairs to prematurely enter telogen, leading to diffuse shedding two to three months later. The condition is self‑limiting; most individuals see regrowth within six months once the underlying stressor resolves.
- Physical trauma from the incision or positioning during long procedures.
- Fluctuations in thyroid hormones and cortisol levels.
- Side effects of medications administered peri‑operatively.
- Reduced blood flow to the scalp during anesthesia.
Patients often ask, “does anesthesia cause hair loss?” While the anesthetic agents themselves are not directly toxic to follicles, the systemic stress response they provoke can initiate telogen effluvium. Similarly, questions like “can anesthesia cause hair thinning?” are answered by recognizing that the hair loss is usually temporary and resolves as the body returns to baseline.
The Role of Weight Changes and Nutrition After Surgery
Weight loss—whether intentional after bariatric surgery or unintentional due to postoperative recovery—has a strong correlation with hair loss after operation. Rapid reductions in caloric intake can deplete essential nutrients that support keratin production, leading to a condition often referred to as “shock hair.”
Weight Loss and Hair Loss Connection
When the body enters a catabolic state, it prioritizes vital organ function over hair growth. Proteins, iron, zinc, and biotin become scarce, and the hair follicle responds by entering the resting phase. This explains why patients report “hair loss after bariatric surgery” or “hair loss after gastric surgery” within weeks of the procedure.
| Weight‑Loss Method | Typical Nutrient Deficiency | Impact on Hair |
|---|---|---|
| Very Low‑Calorie Diet (VLCD) | Protein, Iron, Zinc | Diffuse thinning, increased shedding |
| Bariatric Surgery (Sleeve, Bypass) | Biotin, Vitamin D, B‑Complex | Telogen effluvium, slower regrowth |
| Rapid Fat‑Loss Programs | Essential fatty acids | Hair brittleness, breakage |
Addressing these deficiencies early—through balanced meals, supplementation, and regular monitoring—can dramatically reduce the severity of post‑operative hair loss. Many patients wonder, “does weight loss cause hair loss?” The answer is a qualified yes, but the effect is reversible with proper nutritional support.
When Hair Loss Persists: Identifying Underlying Conditions
While most cases of hair loss after operation resolve within six months, a subset of patients experience prolonged shedding that may signal deeper health issues. Persistent thinning can be linked to hormonal imbalances, autoimmune reactions, or medication side effects.
Hormonal Shifts and Medication Effects
Procedures that affect endocrine organs—such as thyroidectomy or parathyroid surgery—can disrupt hormone levels that regulate hair cycles. Patients often ask, “will my hair grow back after parathyroid surgery?” The answer depends on whether the hormonal balance is restored post‑operatively.
- Thyroid disorders: Hypothyroidism can cause coarse, dry hair and increased shedding.
- Steroid use: High‑dose corticosteroids may trigger alopecia areata‑like patterns.
- Antibiotics and anticoagulants: Certain drugs interfere with nutrient absorption, exacerbating hair loss.
In addition, systemic inflammation after major surgeries can trigger an autoimmune response known as “post‑surgical alopecia,” a rare but documented phenomenon. If shedding continues beyond the typical recovery window, a dermatologist should evaluate for conditions such as alopecia areata, telogen effluvium secondary to chronic illness, or even nutritional deficiencies not addressed by diet alone.
Strategies to Minimize and Manage Hair Loss After Operation
Proactive care can significantly reduce the impact of hair loss after operation. Combining gentle scalp hygiene, targeted supplementation, and lifestyle adjustments creates an environment conducive to regrowth.
Scalp Care and Supplements
Gentle cleansing with sulfate‑free shampoos prevents irritation while maintaining natural oils. Scalp massage stimulates micro‑circulation, encouraging follicular health. When it comes to supplementation, evidence supports the following nutrients:
- Biotin (Vitamin B7): Supports keratin synthesis; 5 mg daily is commonly recommended.
- Iron: Essential for hemoglobin; deficiency is a leading cause of diffuse thinning.
- Zinc: Plays a role in DNA repair and cell division within follicles.
- Omega‑3 fatty acids: Reduce inflammation and improve scalp moisture.
Patients often search “vitamins for hair loss after surgery” and should prioritize a balanced multivitamin that addresses these key elements. Additionally, stress‑reduction techniques—such as mindfulness, moderate exercise, and adequate sleep—help keep cortisol levels in check, further mitigating telogen triggers.
Topical agents like minoxidil can be introduced after the surgical wound has fully healed (usually 4–6 weeks). While not a cure, minoxidil prolongs the anagen phase, giving follicles a better chance to produce visible hair during the recovery period.
When to Consider a Hair Restoration Procedure
If shedding persists beyond a year or if you have pre‑existing thinning that was exacerbated by surgery, a hair restoration solution may be appropriate. Modern techniques such as Follicular Unit Extraction (FUE) and Direct Hair Implantation (DHI) provide natural‑looking results with minimal downtime.
FUE vs. DHI: Choosing the Right Method
| Technique | Procedure Details | Recovery Time | Ideal Candidates |
|---|---|---|---|
| FUE | Individual follicles are harvested using a micro‑punch and implanted. | 7‑10 days for mild swelling; full results in 12‑18 months. | Patients seeking precision and low scarring. |
| DHI | Follicles are loaded into a Choi implanter pen for direct placement. | 5‑8 days for mild swelling; faster graft survival. | Those desiring higher density in a single session. |
Both methods are performed under local anesthesia, eliminating the systemic stress that contributed to the original hair loss. A thorough pre‑operative assessment ensures that any residual effects of previous surgeries—such as altered blood flow or scar tissue—are accounted for, maximizing graft survival.
Why Choose Gold City Hair
At Gold City Hair, we combine more than a decade of expertise in hair restoration with a personalized, transparent approach. Our clinic in Turkey offers state‑of‑the‑art FUE and DHI procedures performed by board‑certified surgeons who understand the unique challenges faced by patients recovering from other operations. We prioritize patient education, detailed pre‑operative planning, and post‑procedure support to ensure lasting confidence and natural results.
Ready to restore your hair and confidence? Contact Gold City Hair today to schedule a confidential consultation and discover a tailored solution that fits your post‑surgical needs.
FAQ
Does anesthesia cause hair loss?
Anesthesia itself isn’t directly toxic to hair follicles, but the stress response it triggers can initiate telogen effluvium.
Can weight loss cause hair loss after surgery?
Yes, rapid weight loss after surgery can lead to nutrient deficiencies that trigger hair shedding.
How long does post‑surgical hair shedding usually last?
Typical telogen effluvium after surgery lasts 3‑6 months, with regrowth beginning around the six‑month mark.
When should I see a dermatologist for hair loss after operation?
If hair shedding persists beyond six months or you notice other symptoms like scalp inflammation, consult a dermatologist.
What supplements are most effective for post‑surgical hair loss?
Biotin, iron, zinc, and omega‑3 fatty acids are the key nutrients that support regrowth after surgery.
Is it safe to use minoxidil after surgery?
Minoxidil can be started once the surgical wound has fully healed, typically after 4‑6 weeks.
What is the difference between FUE and DHI for post‑operative patients?
FUE harvests follicles with a micro‑punch, while DHI uses a Choi implanter pen for direct placement, offering slightly faster graft survival.