Manage vaginal folliculitis with the best soothing relief steps. Learn incredible ways to heal sensitive skin and prevent painful infections.
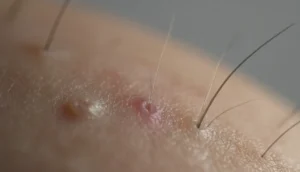
Genital skin conditions can cause a lot of discomfort and worry. Relief is available for those dealing with folliculitis in the pubic area. This common issue is marked by inflamed hair follicles.
Things like hair removal, tight clothes, or infections can trigger folliculitis. It leads to red bumps, itching, and discomfort. Knowing the causes and symptoms is key to treating it effectively.
By figuring out the cause and picking the right treatment, people can regain their comfort and confidence. Our expert advice will guide you through this journey and help you find relief.
Key Takeaways
Identify the underlying cause of genital folliculitis
Choose the right treatment approach for relief
Understand the causes and symptoms of folliculitis
Regain comfort and confidence with effective treatment
Navigate the treatment process with expert guidance
Understanding Vaginal Folliculitis and Its Causes
It’s important to know what causes vaginal folliculitis to treat and prevent it. Vaginal folliculitis is when hair follicles in the genital area get inflamed. This can be painful and uncomfortable.
What Is Genital Folliculitis?
Genital folliculitis is when hair follicles in the pubic area get inflamed, often from infection. It can show up as red bumps or pustules around the hair follicles. This causes discomfort and itching.
The inflammation is usually from bacterial or fungal infections. Staphylococcus aureus and Candida are common causes.
Common Causes and Pathogens
Several factors can lead to folliculitis in the genital area. Bacterial and fungal infections are the main culprits. Staphylococcus aureus is a common bacterium that causes it. Candida can also cause infections, often in people with weak immune systems or too much moisture in the genital area.
Bacterial infections, such as those caused by Staphylococcus aureus
Fungal infections, including Candida
Friction from tight clothing
Poor shaving techniques
Ingrown hairs
Risk Factors You Should Know
Some factors can make you more likely to get vaginal folliculitis. These include:
Wearing tight clothing that causes friction
Shaving or waxing the pubic area, which can lead to ingrown hairs and irritation
Having a compromised immune system, making it harder for the body to fight off infections
Poor hygiene practices, which can lead to the accumulation of bacteria and fungi
Knowing these causes and risk factors helps prevent vaginal folliculitis. Good hygiene, avoiding tight clothing, and proper shaving techniques are key.
Recognizing and Treating Vaginal Folliculitis at Home
Vaginal folliculitis can be uncomfortable. Knowing its symptoms is key to treating it. By recognizing these signs, you can manage it at home.
Identifying the Symptoms
Spotting the signs of vaginal folliculitis is important. Look out for red bumps, pustules, and itching in the genital area. You might also feel pain or tenderness. If you see these signs, act quickly to manage the condition.
Warm Compresses and Gentle Cleansing
Warm compresses can help reduce inflammation and aid in healing. Clean the area gently with mild soap and lukewarm water. Stay away from harsh or abrasive cleansers that can make things worse.
Over-the-Counter Treatments
OTC treatments can help with vaginal folliculitis symptoms. Topical creams or ointments with tea tree oil or hydrocortisone can lessen inflammation and itching. Sometimes, oral antibiotics are needed, but you’ll need a doctor’s prescription for those.
Medical Treatments for Persistent Vaginal Folliculitis
When home treatments don’t work for vaginal folliculitis, it’s time to see a doctor. This is to stop the problem from getting worse and to help it heal.
When to See a Doctor
If you notice any of these signs, you should go to a healthcare professional: folliculitis on the genital area that won’t go away, more redness, swelling, or pus; fever; or if it doesn’t get better with home care. Seeing a doctor early can stop the infection from spreading and prevent scarring.
Persistent or severe symptoms
Increased redness or swelling
Fever or chills
No improvement with home care
Prescription Antibiotics and Antifungals
Doctors might give you antibiotics or antifungals for folliculitis vaginal caused by bacteria or fungus. These medicines aim to get rid of the infection and stop it from coming back.
Some common treatments include:
Oral antibiotics for bacterial folliculitis
Topical antifungals for fungal infections
Combination therapies for mixed infections
Procedures for Severe Cases
For serious folliculitis genital male or female folliculitis, more steps might be needed. This could be draining abscesses or laser hair removal to avoid future problems.
It’s key to listen to your doctor’s advice during these treatments. This ensures they are safe and work well.
Getting medical help when needed can help manage folliculitis after sex or other reasons. It reduces pain and stops long-term issues.
Conclusion: Prevention Strategies for Long-Term Relief
Preventing vaginal folliculitis is key for long-term relief and health. Simple yet effective strategies can lower the risk of folliculitis in the groin and genitals.
Avoiding tight clothing is important. It can cause friction and irritation, leading to folliculitis on the groin. Good hygiene is also vital in preventing folliculitis in the pubic region.
Gentle hair removal methods can help reduce the risk of folliculitis in the private area. Being mindful of these factors and taking proactive steps can lead to lasting relief from vaginal folliculitis.
Creating a personalized prevention plan with expert guidance is beneficial. It helps maintain healthy skin and prevents future folliculitis. With the right strategies, long-term relief is possible.
FAQ
What are the best postpartum vitamins for hair loss
Look for vitamins with biotin, iron, zinc, vitamin D, B‑complex, vitamin C, and collagen to support hair regrowth after childbirth
Can postpartum hair loss be stopped with vitamins
Vitamins help support and nourish hair growth, but they don’t stop shedding instantly—natural postpartum shedding usually resolves on its own
Are Baby Blues Postpartum Hair Vitamins effective
Supplements like Baby Blues may help if they provide key nutrients, but effectiveness varies by individual and nutritional needs
How long does it take to see results from postpartum hair loss vitamins
Most people notice improvements in 8–12 weeks of consistent intake
Can I take postpartum hair loss vitamins while breastfeeding
Many vitamins are safe during breastfeeding, but check with your healthcare provider to ensure they match your needs
What is the role of estrogen in postpartum hair loss
After pregnancy, estrogen levels drop, triggering telogen effluvium—a temporary shedding phase that causes hair loss
Can I take vitamin D for postpartum hair loss
Yes, vitamin D supports hair follicle health, especially if levels are low, but confirm dosage with your doctor
Are there any other nutrients I should take with postpartum hair loss vitamins
Yes—iron, zinc, omega‑3 fatty acids, B vitamins, and collagen all support stronger, healthier hair growth
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC6513076/