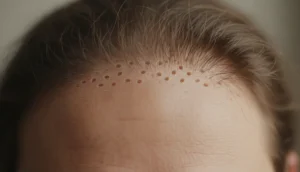
When you wonder what does hair loss from stress look like, the answer lies in the visible patterns and underlying mechanisms that become evident on the scalp. Stress can trigger a range of shedding behaviors, from diffuse thinning to sudden bald spots, and recognizing these signs early can prevent permanent damage. In fact, up to 30% of patients reporting sudden hair thinning cite recent high‑stress events as a primary trigger.
This article explores the visual cues of stress‑related hair loss, explains the biological pathways involved, and outlines how to differentiate it from other forms of alopecia. Whether you are experiencing a few extra strands each day or noticing larger patches, understanding the root cause empowers you to take the right steps toward recovery.
We will cover the typical appearance of stress‑induced shedding, the role of telogen effluvium, how to distinguish it from conditions such as alopecia areata, when professional assessment is essential, and the treatment options available—including advanced hair‑restoration techniques offered by Gold City Hair.
Typical Visual Signs of Stress‑Related Hair Loss

Stress‑related hair loss often follows a recognizable pattern that differs from genetic or hormonal causes. The most common visual indicators include:
- Diffuse thinning across the entire crown rather than a receding hairline.
- Increased shedding when washing, brushing, or after a shower.
- Small, round bald spots that may appear suddenly (often confused with alopecia areata).
- Hair that feels finer or softer than before, indicating a shift in the growth cycle.
- Visible “exclamation‑point” hairs—short, broken strands that emerge from the scalp.
These signs usually emerge 2–3 months after a major stressful event, such as a job loss, illness, or emotional trauma. The delay occurs because stress pushes a large number of hair follicles into the telogen (resting) phase, and they are shed synchronously during the normal shedding cycle.
How Stress Triggers Telogen Effluvium and Other Types
Telogen effluvium is the most common form of stress‑induced hair loss. Under normal conditions, only about 10% of hairs are in the telogen phase. When the body experiences acute or chronic stress, hormonal imbalances (particularly cortisol) cause a larger proportion—sometimes up to 30%—to enter telogen simultaneously. After a few weeks, these hairs are shed, creating the appearance of rapid thinning.
Other, less frequent stress‑related conditions include:
| Condition | Typical Trigger | Hair Appearance | Duration |
|---|---|---|---|
| Telogen Effluvium | Acute emotional or physical stress | Diffuse thinning, shedding of 10–30 hairs per day | 3–6 months, often reversible |
| Alopecia Areata | Autoimmune response, sometimes stress‑related | Round bald patches, “exclamation‑point” hairs | Variable; can become chronic |
| Trichotillomania | Compulsive hair pulling linked to anxiety | Irregular patches, broken hairs of varying lengths | Ongoing until behavior changes |
Understanding these mechanisms helps clinicians decide whether the loss is likely to resolve on its own or if intervention is required. While telogen effluvium usually improves once the stressor is removed, persistent cases may need medical support.
Differentiating Stress‑Induced Shedding from Other Alopecia
Because stress can mimic other hair‑loss disorders, accurate diagnosis is essential. Below are key factors to consider when distinguishing stress‑related shedding from conditions such as alopecia areata or pattern baldness.
- Onset timing: Stress‑induced loss appears 2–3 months after a stressful event; alopecia areata often has a sudden onset without a clear trigger.
- Pattern: Diffuse thinning is typical for telogen effluvium, whereas alopecia areata creates well‑defined, round patches.
- Hair shaft quality: In telogen effluvium, shed hairs are uniform and lack the “exclamation‑point” morphology seen in alopecia areata.
- Associated symptoms: Autoimmune conditions may present with nail pitting or skin changes, which are absent in pure stress‑related loss.
Diagnostic tools such as a scalp‑pull test, trichoscopy, and blood work (to assess thyroid function, iron levels, and cortisol) assist dermatologists in confirming the cause. When the primary driver is stress, addressing lifestyle factors often yields the best results.
When to Seek Professional Help and Diagnostic Steps
If you notice any of the following, it is advisable to schedule a consultation with a hair‑restoration specialist:
- Shedding more than 100 hairs per day for consecutive weeks.
- Sudden appearance of bald patches larger than a coin.
- Accompanying symptoms such as scalp itching, redness, or pain.
- Persistent thinning despite reduced stress levels.
- Family history of autoimmune disorders or unexplained hair loss.
During the appointment, the clinician will typically perform:
- Medical history review to identify recent stressors, medications, and nutritional factors.
- Physical examination including a scalp‑pull test to quantify active shedding.
- Trichoscopic analysis to visualize follicle health and detect signs of inflammation.
- Laboratory tests for thyroid hormones, iron, vitamin D, and cortisol levels.
These steps help rule out other causes such as alopecia, hormonal imbalances, or chronic illnesses, ensuring that any treatment plan targets the correct underlying issue.
Treatment Options and Long‑Term Management
While stress‑related shedding often resolves once the trigger is managed, several interventions can accelerate recovery and improve scalp health.
Stress Management and Lifestyle Adjustments
- Regular physical activity (30 minutes most days) to lower cortisol.
- Mind‑body practices such as meditation, yoga, or deep‑breathing exercises.
- Balanced diet rich in protein, iron, zinc, and vitamins A, C, D, and E.
- Adequate sleep (7–9 hours) to support hair‑follicle regeneration.
Medical Therapies
Topical minoxidil, oral finasteride (for men), and low‑dose oral corticosteroids can shorten the telogen phase and promote regrowth. In cases where an autoimmune component is suspected, topical or intralesional corticosteroids may be prescribed.
Advanced Hair Restoration at Gold City Hair
If hair density does not improve after six months of conservative measures, Gold City Hair offers state‑of‑the‑art procedures such as:
- Follicular Unit Extraction (FUE) – Individual follicles are harvested and implanted with minimal scarring.
- Direct Hair Implantation (DHI) – Uses a patented pen‑style device for precise placement and higher graft survival.
- Eyebrow and Beard Transplants – Tailored solutions for facial hair restoration.
All procedures are performed by experienced surgeons in Turkey, with transparent communication and personalized after‑care plans designed to maximize natural‑looking results.
Why Choose Gold City Hair
Gold City Hair combines cutting‑edge technology with a patient‑centered approach. Since 2017, the clinic has delivered successful hair‑restoration outcomes using FUE, DHI, and facial‑hair transplantation techniques. Each treatment plan is customized to address the unique cause of hair loss, whether stress‑related shedding or genetic alopecia. Transparent communication, comprehensive pre‑operative assessments, and post‑procedure support ensure confidence and satisfaction throughout the journey.
Ready to restore a fuller, healthier head of hair? Contact Gold City Hair today for a personalized evaluation and discover how our expert team can help you regain confidence.
FAQ
What does hair loss from stress look like?
Stress‑related hair loss usually appears as diffuse thinning across the crown, increased shedding during washing, and occasional round bald spots.
How does telogen effluvium cause hair shedding?
Telogen effluvium forces a large percentage of hair follicles into the resting phase, leading to synchronized shedding weeks later.
How can I differentiate stress‑induced hair loss from alopecia areata?
Stress‑induced loss is diffuse and appears months after stress, while alopecia areata shows sudden, well‑defined round patches with exclamation‑point hairs.
When should I see a dermatologist for stress‑related hair loss?
Seek professional help if you shed over 100 hairs daily, develop large bald patches, experience scalp symptoms, or the thinning persists despite stress reduction.
What treatment options are available for stress‑induced hair loss?
Options include stress management, nutritional support, topical minoxidil, oral finasteride (for men), low‑dose corticosteroids, and advanced hair‑restoration procedures if needed.
Can hair transplant help with stress‑related thinning?
Yes, if the thinning is permanent after the stressor resolves, transplant procedures like FUE or DHI can restore density.
How long does stress‑induced hair loss typically last?
Most cases resolve within 3–6 months after the stressor is removed, though some may persist longer and need treatment.
What lifestyle changes can reduce stress‑related hair loss?
Regular exercise, mindfulness practices, balanced nutrition, adequate sleep, and avoiding harsh hair treatments can mitigate shedding.