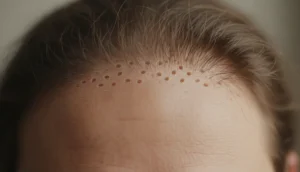
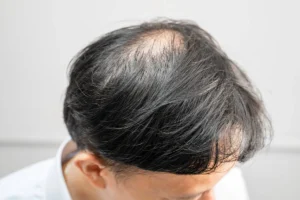
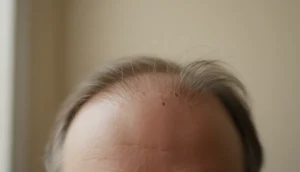
Autoimmune hair loss in women is a complex condition where the immune system mistakenly attacks hair follicles, leading to sudden shedding and thinning. Understanding why this happens, how it is diagnosed, and which treatments work best can empower you to take control of your hair health. Each year, thousands of women experience this distressing form of alopecia, often feeling isolated and uncertain about their options.
In this article, we explore the underlying triggers, the diagnostic process, and the most effective medical and surgical solutions, including the role of hair transplant techniques such as FUE and DHI offered by Gold City Hair. Whether you are dealing with patchy bald spots or diffuse thinning, the information below will help you navigate the journey toward regrowth and confidence.
We will also discuss lifestyle adjustments that support hair regrowth, and clarify when a transplant may be a viable long‑term solution. Let’s begin by uncovering the root causes of this autoimmune condition.
What Triggers Autoimmune Hair Loss in Women?
Autoimmune hair loss in women often manifests as alopecia areata, a condition where the immune system targets the hair follicle’s growth phase. While the exact cause remains elusive, several factors increase the risk of developing this disorder.
Alopecia Areata and Related Forms
Alopecia areata is the most common presentation, characterized by round, smooth patches of hair loss. In some cases, it progresses to alopecia totalis (loss of all scalp hair) or alopecia universalis (loss of all body hair). Women may also experience telogen effluvium triggered by systemic autoimmune activity, leading to diffuse thinning.
Other Autoimmune Conditions
- Hashimoto’s thyroiditis – thyroid hormone imbalance can exacerbate hair shedding.
- Lupus erythematosus – systemic inflammation often includes scalp involvement.
- Vitiligo – shared autoimmune pathways may affect melanocytes and hair follicles.
Genetic and Environmental Influences
Family history plays a significant role; genes that regulate immune tolerance can predispose individuals to autoimmune attacks on hair. Environmental triggers such as viral infections, severe stress, or hormonal fluctuations (e.g., pregnancy, menopause) can also initiate or worsen the condition.
Recognizing these triggers is essential for targeted therapy and for minimizing future flare‑ups.

How Is Autoimmune Hair Loss Diagnosed?
Accurate diagnosis distinguishes autoimmune hair loss from other forms such as androgenetic alopecia or mechanical damage. Dermatologists employ a combination of clinical observation, laboratory testing, and sometimes scalp biopsies.
Clinical Examination
The physician first inspects the scalp for characteristic signs: smooth, round bald patches, exclamation‑mark hairs at the margins, and occasional “yellow dots” under dermoscopy. A detailed medical history helps identify associated autoimmune disorders.
Blood Tests
Blood work screens for underlying systemic issues. Common panels include:
- Thyroid function tests (TSH, free T4)
- Antinuclear antibody (ANA) profile
- Anti‑thyroid peroxidase (TPO) antibodies
- Inflammatory markers (CRP, ESR)
Scalp Biopsy
When the diagnosis remains uncertain, a 4‑mm punch biopsy provides histological confirmation. The sample reveals perifollicular lymphocytic infiltrates typical of autoimmune activity.
| Diagnostic Method | Purpose | Typical Findings |
|---|---|---|
| Clinical Examination | Initial assessment | Patchy bald spots, exclamation‑mark hairs |
| Blood Tests | Identify systemic autoimmune links | Elevated antibodies, thyroid imbalance |
| Scalp Biopsy | Confirm follicular inflammation | Lymphocytic infiltrate around hair bulbs |
Combining these tools ensures a precise diagnosis, guiding the most effective treatment plan.
Effective Treatment Options for Autoimmune Hair Loss
Therapeutic strategies aim to suppress the misguided immune response, stimulate follicular regrowth, and, when appropriate, restore density through transplantation. Treatment choice depends on disease severity, patient age, and personal preferences.
Topical and Oral Medications
- Corticosteroid injections – Directly reduce inflammation in active patches.
- Topical corticosteroids (e.g., clobetasol) – Useful for limited areas.
- Oral corticosteroids – Short‑term courses for extensive disease.
- JAK inhibitors (tofacitinib, ruxolitinib) – Emerging oral agents showing promising regrowth rates.
- Anthralin and minoxidil – Adjuncts that promote blood flow and follicle activation.
Light and Laser Therapies
Low‑level laser therapy (LLLT) and excimer laser treatments can modulate immune activity while enhancing cellular metabolism, offering a non‑invasive complement to medication.
When Hair Transplant Becomes an Option
For women whose autoimmune condition has stabilized and who have permanent follicular loss, a hair transplant can provide lasting density. Techniques such as Follicular Unit Extraction (FUE) and Direct Hair Implantation (DHI) are performed under local anesthesia, yielding natural‑looking results with minimal downtime.
Before proceeding, patients must undergo a thorough evaluation to confirm that the disease is inactive, as active autoimmune attacks can jeopardize graft survival.
Lifestyle and Home Care Strategies to Support Hair Regrowth
Medical treatment works best when paired with supportive daily habits. Simple adjustments can reduce inflammation, improve scalp health, and enhance the effectiveness of prescribed therapies.
Nutrition for Hair Health
- Protein‑rich foods (lean meats, legumes) – Provide essential amino acids for keratin production.
- Omega‑3 fatty acids (salmon, flaxseed) – Reduce systemic inflammation.
- Biotin, zinc, and iron – Deficiencies are linked to increased hair shedding.
- Antioxidant‑rich fruits and vegetables – Combat oxidative stress that may trigger autoimmunity.
Stress Management
Chronic stress elevates cortisol, which can exacerbate autoimmune activity. Techniques such as mindfulness meditation, yoga, and regular aerobic exercise have been shown to lower stress hormones and may improve hair outcomes.
Gentle Hair Care Practices
- Avoid tight hairstyles that pull on the scalp.
- Use sulfate‑free, mild shampoos to prevent irritation.
- Limit heat styling and harsh chemical treatments.
- Pat hair dry instead of vigorous rubbing.
Adopting these habits creates a scalp environment conducive to regrowth and helps maintain the results of medical interventions.
When to Consider a Hair Transplant for Autoimmune Hair Loss
Even with optimal medical therapy, some women experience permanent follicular loss that does not respond to conventional treatments. In such cases, a hair transplant offers a realistic path to restoring density and confidence.
Eligibility Criteria
- Stable disease for at least 12 months (no active inflammation).
- Adequate donor hair density in the occipital region.
- Realistic expectations regarding results and maintenance.
Procedure Options
| Technique | Key Advantages | Typical Recovery Time |
|---|---|---|
| FUE (Follicular Unit Extraction) | Minimally invasive, no linear scar, precise graft placement | 7‑10 days for mild swelling |
| DHI (Direct Hair Implantation) | Higher graft survival, faster implantation, natural angle | 5‑8 days for mild discomfort |
Gold City Hair’s experienced team customizes the transplant plan, ensuring that grafts are harvested from healthy, unaffected donor zones and implanted at the correct depth and angle for a natural look.
Why Choose Gold City Hair for Your Hair Restoration Journey
Gold City Hair has been delivering personalized hair restoration solutions in Turkey since 2017. Our clinic combines state‑of‑the‑art FUE and DHI techniques with a compassionate, transparent approach. Every patient receives a thorough assessment, a customized treatment plan, and ongoing support throughout the recovery process. With a focus on safety, natural results, and patient confidence, Gold City Hair is a trusted partner for women seeking lasting solutions to autoimmune hair loss.
Ready to reclaim your confidence and restore a fuller head of hair? Contact Gold City Hair today to schedule a personalized consultation and explore the most effective treatment pathway for you.
Take the first step toward lasting regrowth—your journey starts now.
FAQ
What causes autoimmune hair loss in women?
Autoimmune hair loss in women is triggered by the immune system attacking hair follicles, often linked to alopecia areata, thyroid disorders, lupus, vitiligo, genetics, and environmental stressors.
How is autoimmune hair loss diagnosed?
Diagnosis combines clinical examination, blood tests for autoimmune markers, and sometimes a scalp biopsy to confirm follicular inflammation.
What treatment options are available for autoimmune hair loss?
Treatments include topical and oral corticosteroids, JAK inhibitors, anthralin, minoxidil, low‑level laser therapy, and, when appropriate, hair transplantation.
When is a hair transplant appropriate for women with autoimmune hair loss?
A transplant is considered when the disease has been stable for at least 12 months, there is sufficient donor hair, and the patient has realistic expectations.
Can lifestyle changes help improve hair regrowth in autoimmune alopecia?
Yes, balanced nutrition, stress reduction, and gentle hair care can support regrowth and enhance treatment effectiveness.
What are the differences between FUE and DHI hair transplant techniques?
FUE extracts individual follicles with minimal scarring, while DHI implants grafts directly using a specialized pen for higher survival and natural angle.